 The more risks you have, the greater your chances of experiencing a blood clot. The combination of long-distance travel with one or more of these risks may increase the likelihood of developing a blood clot. Limited mobility (for example, a leg cast).Active cancer or recent cancer treatment.Previous blood clot or a family history of blood clots.Pregnancy and the postpartum period (up to 3 months after childbirth).Hormone replacement therapy (medical treatment in which hormones are given to reduce the effects of menopause).Use of estrogen-containing contraceptives (for example, birth control pills, rings,patches).Recent surgery or injury (within 3 months).Obesity ( body mass index greater than 30kg/m 2).Older age (risk increases after age 40).Most people who develop travel-associated blood clots have one or more other risks for blood clots, such as: Your level of risk depends on the duration of travel as well as whether you have any other risks for blood clots. Understand What Can Increase Your Risk for Blood ClotsĮven if you travel a long distance, the risk of developing a blood clot is generally very small. The good news is there are things you can do to protect your health and reduce your risk of blood clots during a long-distance trip. This is called a pulmonary embolism, and it may be fatal. However, a serious health problem can occur when a part of the blood clot breaks off and travels to the lungs causing a blockage. Many times the blood clot will dissolve on its own. The longer you are immobile, the greater is your risk of developing a blood clot. If a blood clot is large or there are many clots, a pulmonary embolism can cause death.Blood clots can form in the deep veins (veins below the surface that are not visible through the skin) of your legs during travel because you are sitting still in a confined space for long periods of time. This can be especially serious in the case of a pulmonary embolism, which blocks blood flow to the lungs. Without treatment, VTE can restrict or block blood flow and oxygen, which can damage the body’s tissue or organs. If you have VTE, your provider may prescribe medicines to treat serious vein blockages and help prevent further blood clots from forming. 
Your provider will do tests to find out whether you have the condition. If you have recently had surgery or have other risk factors of VTE, talk to your healthcare provider about your risk and how to prevent blood clots. Sometimes VTE occurs without any obvious signs, which can make it harder to diagnose. A pulmonary embolism can cause sudden chest pain and shortness of breath. Swelling, redness, and pain are some of the symptoms of DVT. Inflammation and serious infection also raise the likelihood of blood clots. 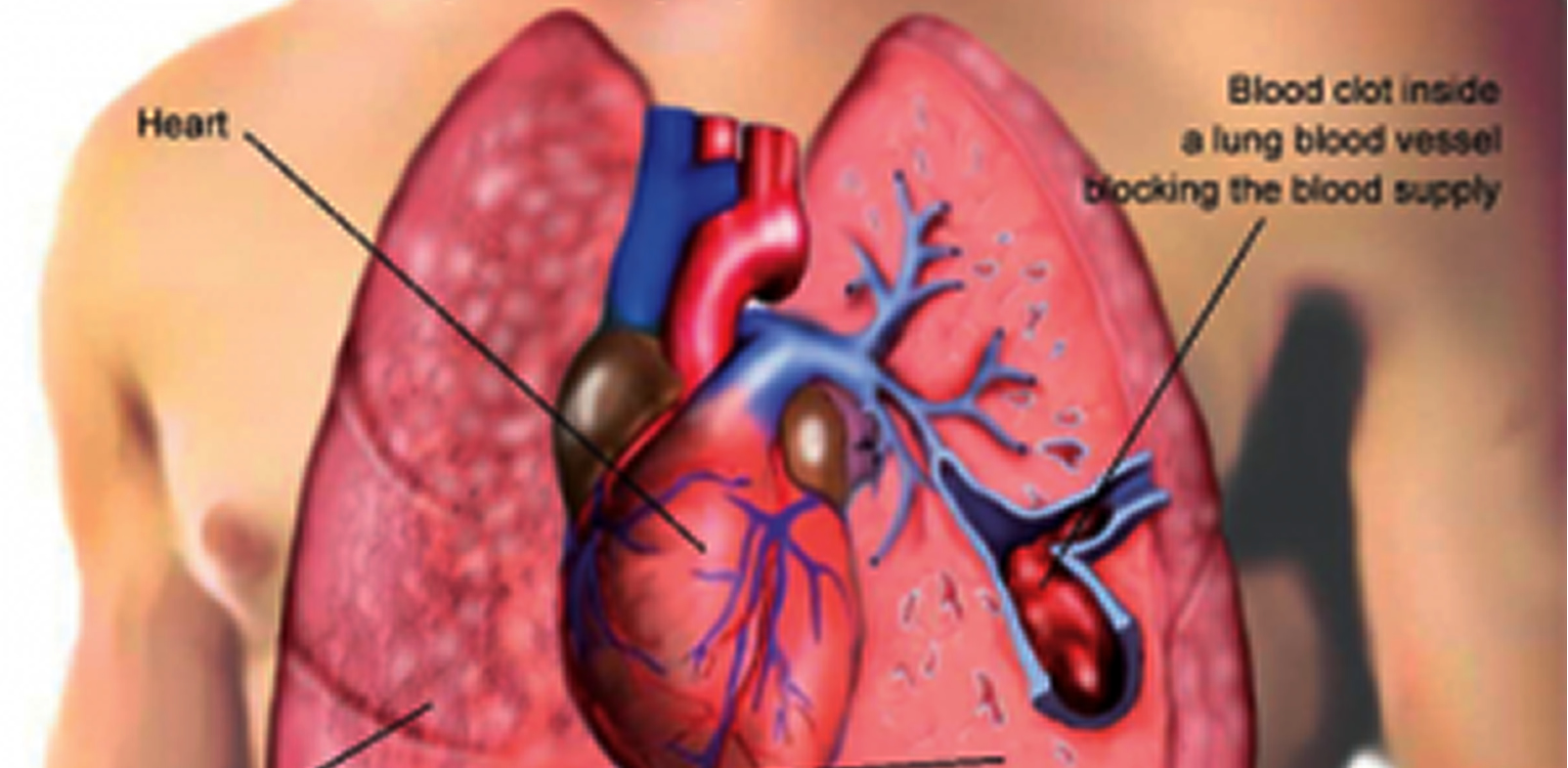
Lack of movement after surgery or while traveling long distances can raise the likelihood of blood clotting. This is because blood clots can develop in veins damaged by surgery or injury. The risk of developing VTE is highest after major surgery, major injury, or during periods of infection and inflammation. As many as 600,000 VTE events occur each year in the United States. Pulmonary embolism occurs when a clot breaks loose and travels through the bloodstream to the lungs. DVTs can also occur in the arms, especially if there is a large intravenous central line in the vein. DVT occurs when a blood clot forms in a deep vein, usually in the lower leg, thigh, or pelvis. VTE includes deep vein thrombosis (DVT) and pulmonary embolism (PE). Venous thromboembolism (VTE) is a condition that occurs when a blood clot forms in a vein. 
Medical Animation Copyright © 2022 Nucleus Medical Media, All rights reserved. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
